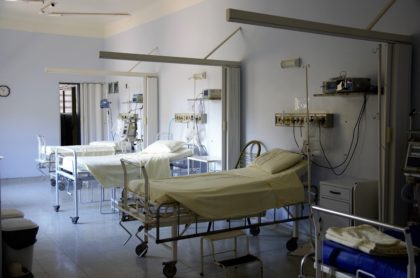
Over the past two years, you’ve probably heard more about hospital bed availability than you may have expected to hear in your entire life. Tracking total hospital beds and ICU beds occupied has helped communities know when to increase mitigation to preserve those limited resources. With expanding SARS-CoV-2 immunity through vaccination and prior infection, we can hope to hear less about strained healthcare facilities; already we saw that the combination of immunity and a less severe strain in Omicron BA.1 meant less demand for ICU beds. It’s worth remembering though that when we talk about hospital beds, we’re talking about more than furniture and equipment. A hospital may have a physical bed, but without physicians and nurses to care for the patient in the bed, it doesn’t count. And with fewer clinicians now than two years ago, the US healthcare system may experience lingering effects of the pandemic even when there are few COVID-19 patients to treat.
Long COVID is the much-discussed but not fully understood experience of persistent symptoms months after initial infection, possibly without any actual virus present in one’s body. Maybe we also need a “long pandemic” concept to describe the long-term community impacts independent of transmission levels. After nearly a decade of growth, the number of hospital employees decreased and then held steady at a plateau lower than the peak, as shown by Bureau of Labor statistics. Although that chart does not distinguish clinical and administrative staff, the psychological toll on clinicians and reports of nursing shortages indicate that is not purely a reduction in administrative staff. Between the trauma of having to deal with gravely ill patients, needing to work overtime to staff those beds, and the risk to their own health due to constant potential for exposure, it is little wonder that some physicians and nurses are experiencing PTSD or similar symptoms and opting to retire or seek other forms of employment. And that’s before we consider the confrontations with patients and their families over appropriate care and the threats that some healthcare providers and health officials have faced.
Healthcare providers are perhaps the most obvious to be affected, but of course other communities have been and will be impacted as well. For those of you in higher education, you’ve had to relearn how to do your job online and then possibly relearned again to use some form of hybrid of in-person and online teaching. Maybe some of you have had to play of the role of enforcing mask or distancing rules. If you have a research program, most likely it had to be paused for a while and perhaps reimagined afterwards to accommodate new restrictions, not to mention all the conferences that had to be cancelled or virtualized. I’m sure the stress lingers, the career disruptions are still being navigated, and lower enrollment is raising existential questions on some campuses and forcing tough decisions on many others. Obviously I’m in no position to tell you how to fix any of these issues, and I likely overlooked challenges some of you are facing. But I want to at least acknowledge those challenges.
On top of all of that, it’s not as if the virus itself has disappeared. We are effectively transitioning away from a collective response and treating this virus as just another medical concern for each person to assess for themselves. For some that will mean resuming their pre-2020 routines without giving the virus much further thought. For others, that means maintaining the same level of diligence about tracking local numbers and making case-by-case decisions for every errand and social gathering. After weeks of deliberation, my company returned to the office Monday for the first time in over six months, and I had to ignore a vague sense that I should get out of there as quickly as possible. I expect that will pass after the office becomes part of my routine again, but others have experienced more profound isolation and may need more than just time to resume previous activities.

So there’s plenty of work to do ahead to deal with “long pandemic.” Where to start? Fortunately, ESN has arranged for a session with Dr. Broderick Leaks to discuss cultivating good mental health in grad school. You can register for the online event here; it will be held April 25th at 8pm EDT. And if you need more personal care or advice for a domain other than academia, don’t hesitate to contact a counselor or mental health professional.
More generally and non-clinically, I think common sense will tell us that we are going to need a lot of grace for ourselves and each other going forward. We have been through a significant shared experience with dramatically different individual consequences. Some of us will be grieving the loss of family and friends. Others have experienced the loss of opportunities and time, the loss of routines and structures that provide stability and support, or the loss of relationships. The magnitude of those losses may vary, but the emotions can be similar and can hit at odd and unexpected times. And our emotions don’t care if the isolation and missed opportunities were in service of a greater good of protecting the health of our communities. We don’t have to let those emotions dictate all our choices, but they are part of our experience and we need to make space for them so we can handle them appropriately.
In addition to grace, I think we are going to need to work at rebuilding trust. Our trust in each other and in our institutions may have been eroding prior to the pandemic, but the pandemic certainly provided a focal point for testing that trust. And it seems like every day there is a new opportunity to choose sides and reinforce suspicions of some other group. One way we can get off that path is to take the small step of trusting that someone else is worth engaging in conversation rather than writing them off. As a small example, I’d point to the conversation around my last blog post. I appreciated the opportunity to understand the legal side better, and what I felt was an opportunity to have my perspective understood better. I don’t think we resolved all of our points of disagreement, but I think we did manage to get over that initial wariness of even talking to someone who disagrees on such a high profile and charged issue. In the present moment, I’d like to think even that’s worth something.
And finally, since I opened with a look at some practical needs for the future like the need for more clinicians, I want to offer a word of encouragement. As I noted, many of you are in higher education. The solution to many of the “long pandemic” challenges is going to be more young people trained as physicians, as nurses, as public health professionals, as educators, and as all the other specialties which have been particularly strained over the past two years. Some of you may be in school yourself to fill those jobs. Others of you are doing the work and having been doing the work to train those future specialists. Still more of you may have a support role somewhere in that pipeline. And some of you are the specialists already in those fields. Wherever you are in that process, whatever role you are playing, if you are involved then let me say thank you on behalf of myself and all of us who are going to need the fruits of your labor in the days and years to come.
Andy has worn many hats in his life. He knows this is a dreadfully clichéd notion, but since it is also literally true he uses it anyway. Among his current metaphorical hats: husband of one wife, father of two teenagers, reader of science fiction and science fact, enthusiast of contemporary symphonic music, and chief science officer. Previous metaphorical hats include: comp bio postdoc, molecular biology grad student, InterVarsity chapter president (that one came with a literal hat), music store clerk, house painter, and mosquito trapper. Among his more unique literal hats: British bobby, captain’s hats (of varying levels of authenticity) of several specific vessels, a deerstalker from 221B Baker St, and a railroad engineer’s cap. His monthly Science in Review is drawn from his weekly Science Corner posts — Wednesdays, 8am (Eastern) on the Emerging Scholars Network Blog. His book Faith across the Multiverse is available from Hendrickson.

Leave a Reply