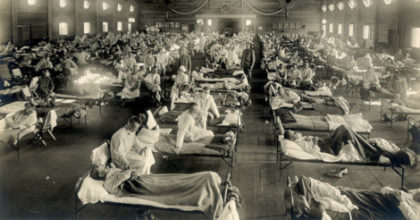
This coming Sunday we will mark 100 years since the armistice that ended World War I. The war shaped global trends for much of the ensuing century; not least of its legacies was the influenza pandemic of 1918 and 1919. Neither humanity’s first nor last widespread encounter with influenza, the 1918-19 pandemic is notable for how quickly and widely it spread: in less than 6 months it was on every continent and ultimately infected as many as 1 out of every 3 people on the planet. Unprecedented troop mobilization meant that young people were gathered together from the corners of many nations, mixed together in groupings that otherwise would have remained hundreds or thousands of miles apart their entire lives, and then sent to distant fronts with crowded living conditions. The war was not solely responsible for the pandemic, and peculiarities of the virus made it especially deadly, but one could scarcely engineer a better scenario for spreading a pathogen.
Exacerbating the deadliness of the virus was the lack of a vaccine or indeed any specific treatment or preventive measures. Good hygiene and social distancing were the main options for effectively reducing the spread; once someone was ill, care could only focus on symptoms and complications. We did not even know what caused influenza in 1918. The existence of any viruses had only been discovered twenty years earlier, and it would be another fifteen years before the influenza virus would be identified. The first vaccine came five years later, in time to inoculate soldiers in World War II, although the efficacy of early vaccines was unclear. The first antiviral drugs for influenza would take another several decades to develop. The virus evolves rapidly, so those drugs are used sparingly to minimize resistance, and the vaccine must be updated every year (PSA: there’s still time to get this year’s vaccine).
Hence the excitement over a new study showing that llama antibodies can protect against a wide variety of influenza viruses. Apparently, llamas can do what we cannot because their antibodies are smaller, allowing them to target inner portions of the virus particles that are more strongly conserved because of functional constraints. That means we may not be able to engineer a vaccine that causes our own immune system to generate antibodies with similar broad coverage–allowing for less frequent vaccine administration–but we may be able to modify the llama antibodies into a treatment.
If llamas are able to provide us a viable treatment, they would be the latest in a series of animals that are part of the influenza story. The virus was first isolated from ferrets, and ferret antibodies continue to be used as reference for assessing which strains to include in the vaccine each year. Chickens and other related fowl seem to be the main reservoirs for influenza, while pigs are often an intermediate host for bird strains to adapt and ultimately become more infectious to humans. We still grow much of the virus needed to make the vaccine in chicken eggs, which is why those with relevant allergies need to be careful about which vaccine they receive. Other animals can also become infected; recently there was evidence of an outbreak among cats that also spread to at least one human. As we have made the world smaller over the past century, we get closer not just to our fellow humans but also all the other living creatures, for better and worse in both directions.
The book club discussion of Faith across the Multiverse continues with Chapter 5; join the conversation at the Peaceful Science forum.
Andy has worn many hats in his life. He knows this is a dreadfully clichéd notion, but since it is also literally true he uses it anyway. Among his current metaphorical hats: husband of one wife, father of two teenagers, reader of science fiction and science fact, enthusiast of contemporary symphonic music, and chief science officer. Previous metaphorical hats include: comp bio postdoc, molecular biology grad student, InterVarsity chapter president (that one came with a literal hat), music store clerk, house painter, and mosquito trapper. Among his more unique literal hats: British bobby, captain’s hats (of varying levels of authenticity) of several specific vessels, a deerstalker from 221B Baker St, and a railroad engineer’s cap. His monthly Science in Review is drawn from his weekly Science Corner posts — Wednesdays, 8am (Eastern) on the Emerging Scholars Network Blog. His book Faith across the Multiverse is available from Hendrickson.

Leave a Reply