After a holiday hiatus, I am resuming my “director’s cut” look at one of my weekly Facebook posts. Look for this feature on the last Wednesday of the month.
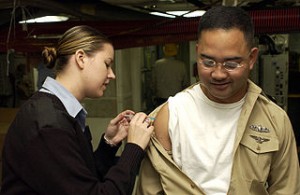
The most discussed topic of the past month was mandatory flu vaccines for healthcare workers. In the midst of a more-severe-than-usual flu season, there have been several stories about nurses losing their jobs for declining the vaccine. We discussed an incident in Indiana reported here and here, and a case from Missouri covered here. In both instances, the nurses cited religious beliefs as contributing to their refusal, with some mention of safety concerns. They felt that they had a right to decide what went into their bodies, and that mandatory vaccination policies conflicted with that right and their religious freedoms.
The Facebook discussion was fairly positive in favor of vaccination. There was a consensus that vaccinating healthcare workers was an important measure for protecting patients and minimizing the spread of disease in healthcare settings, although some folks did stop short of endorsing blanket mandates. One participant noted that these policies are sometimes applied across all hospital departments regardless of the amount of contact with patients; many transcriptionists, chart coders and other administrative personnel work offsite.
Ultimately, the topic of herd immunity was taken up. Herd immunity is the phenomenon where, once enough individuals in a population are vaccinated or immune to an infection, then the population as a whole is immune in a certain sense. At that point, even individuals who never got vaccinated experience some protection. This paper on herd immunity and influenza was cited; it concludes that an 80-90% level of vaccination would be required to achieve herd immunity in most years (both the virus and the vaccine can vary from year to year). This level is far higher than the 50-60% coverage typically achieved in the US.
The talk of herd immunity got me thinking again about the tension over vaccination expressed by the nurses. At the population level, research and public health experience has shown that the benefits to administering vaccines almost always outweigh the risks. But as more and more people receive the vaccine, that risk/benefit calculation for each individual begins to shift. At some point, the risk of side effects to an individual becomes greater than the chance of getting exposed to the disease. As an extreme example, no one is lining up for the smallpox vaccine, even though the virus still exists and thus there is some infinitesimal but nonzero probability of contracting smallpox. And even when the disease is not that rare, one might still be inclined to hope that enough other people will get the vaccine to provide herd immunity in order to avoid even the minimal risk of side effects.
Thus, and I say this as someone trained at a public health school and who makes sure his kids get all the recommended vaccinations, we see that vaccines are not an absolute good. The risks and benefits should be considered in each individual’s context. And if someone has incomplete information or inaccurate information about the risks and benefits, or about the cost of side effects and the cost of getting sick, or about how to accurately reason about the probability of rare events (something science has shown humans to be not very good at, at least innately), then you can start to understand how we can reach different conclusions on a given individual’s need to get a particular vaccination.
And yet we know that if everyone rejects the vaccine, the health outcome for many individuals and for the population will be worse. So, how do we resolve that tension? Presumably education is a component, so everyone is at least starting from the same point when evaluating relative costs. Are vaccination mandates another tool? Is it appropriate to have a policy which says, in essence, that you need to get a vaccine because it is better for us all collectively if you do, even though it involves some risk to you personally? As Christians, should we endorse such policies, since they encourage servanthood and putting the needs of others above our own? Or do such policies undermine the personhood of individuals imbued in them by their Creator?
I also wonder about the appeal to religious freedom. As participants in a secular, pluralistic society, how do we decide whether this is a religious belief meriting protection? We might wish to say that protected religious beliefs must be the teachings of well-known religions. But who decides which ones make the cut? Doesn’t the very notion of deciding represent a restriction on religious freedom? Recall that several states were founded by people whose religious beliefs weren’t accepted by the majority of their society, prompting them to create their own new society where their religion would be tolerated. Isn’t the whole point of the First Amendment to allow people to act their conscience rather than have to adhere to particular pre-approved sets of doctrines? Is there any grounds on which to deny any particular belief, even if it is held by one person?
As I ponder that one, I’m struck with the feeling that we’ve reached a point where “religious beliefs” means “anything one believes strongly without, or in spite of, evidence.” If that’s the case, then it seems hard to deny any particular such belief. Is that where we are? If so, how do we use science to set policy if everyone is entitled to actively ignore some amount of evidence?
About the author:
Andy has worn many hats in his life. He knows this is a dreadfully clichéd notion, but since it is also literally true he uses it anyway. Among his current metaphorical hats: husband of one wife, father of two teenagers, reader of science fiction and science fact, enthusiast of contemporary symphonic music, and chief science officer. Previous metaphorical hats include: comp bio postdoc, molecular biology grad student, InterVarsity chapter president (that one came with a literal hat), music store clerk, house painter, and mosquito trapper. Among his more unique literal hats: British bobby, captain's hats (of varying levels of authenticity) of several specific vessels, a deerstalker from 221B Baker St, and a railroad engineer's cap. His monthly Science in Review is drawn from his weekly Science Corner posts -- Wednesdays, 8am (Eastern) on the Emerging Scholars Network Blog. His book Faith across the Multiverse is available from Hendrickson.
